Sleeve gastrectomy and new stapling technology are both safe and effective approaches to treating obesity, type 2 diabetes, and other related health conditions—so much so that safety data now strongly favors sleeve gastrectomy over any non-surgical treatment. Here’s how sleeve technology continues to improve the state of the art in weight loss and diabetes treatment.
What is Sleeve Gastrectomy
Sleeve gastrectomy, also known as vertical sleeve gastrectomy, is a weight loss surgery that removes critical hormone-producing tissue and reduces the size of the stomach by removing a portion of it. This leads to the change of the metabolic hormone profile controlling body weight and blood sugar, as well as the creation of a smaller stomach pouch, which collectively result in a much lower body weight set point and patients feeling full after eating smaller portions. This procedure is minimally invasive and does not involve rerouting the small intestine, which helps to reduce the risk of complications.
One of the key benefits of sleeve gastrectomy is its safety profile. The procedure is performed using the keyhole approach of laparoscopic techniques, which reduces the risk of complications such as infections, bleeding, and scarring. In addition, the procedure has a low rate of long-term complications, such as malnutrition or vitamin deficiencies, as the majority of the stomach and digestive system remain intact.
Another reason why sleeve gastrectomy is effective is that long term studies show it leads to improved lipid profile, less fat storage in the liver, lower blood sugars and of course, significant weight loss. In most cases, patients can expect to lose 60-70% of their excess weight within the first two years after the procedure. This weight loss not only improves a patient’s overall health, but it can also lead to the resolution of other related health conditions, such as diabetes, high blood pressure, and sleep apnea.
Stapling Technology in Sleeve Gastrectomy
New stapling technology has recently improved the safety and effectiveness of sleeve gastrectomy. The use of new, advanced stapling devices allows for more precise and controlled stapling, which reduces the risk of leaks and bleeding. Additionally, the new devices are designed to reduce postoperative pain and accelerate the recovery process, making the procedure even more appealing to patients. Early studies suggest the advanced stapling technology may also reduce side effects of acid reflux and scar tissue formation within the new stomach. The image below shows how new advanced stapling technology creates a seamless, even staple line every time.
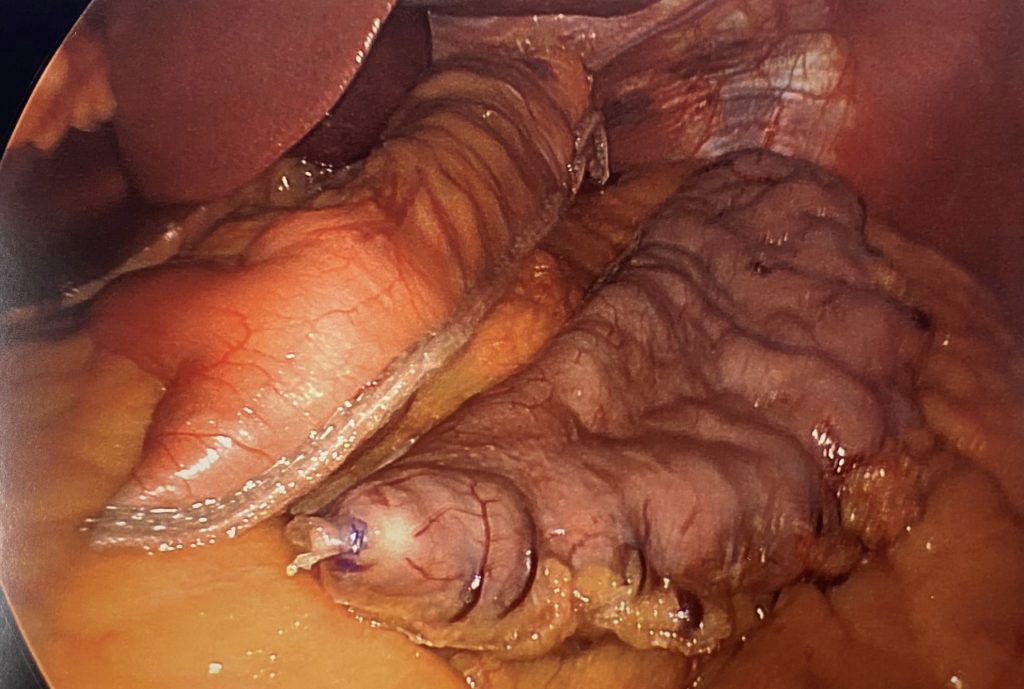
In the image above, to the left is the healthy retained stomach “sleeve”, and to the right is the outer hormonally active stomach tissue that is being removed. Notice the long, straight, clean staple line produced by advanced stapling technology.
The Bottom Line
In conclusion, sleeve gastrectomy and new stapling technology are highly safe and effective methods of treating obesity, type 2 diabetes and related health conditions. The procedure’s minimally invasive nature, low rate of complications, and significant weight loss results make it an attractive option for patients. The use of new stapling technology has further improved the safety and effectiveness of sleeve gastrectomy, making it a highly effective and well-tolerated procedure—one that Medicare, Medicaid, Tricare, and nearly all commercial health insurance plans consider medically necessary with a BMI over 35.




